Unfortunately I can give a first hand description of bunion formation. Having a personal interest I have thoroughly researched this deformity. Hallux is Latin for our big toe and valgus is a deformity that describes a movement of a bone towards the mid-line of the body. This is the same deformity that occurs in ‘knock-kneed’ when the shin bone moves away from the centre of the body. In hallux valgus it is actually the metatarsal bone of the big toe that first moves medially and then the big toe compensates by moving in the opposite direction towards the second toe [Fig. 1]. This causes the charactaristic boney lump at the base of the toe, which is actually the protruding head of the metatarsal bone. Its common name is a bunion.
Bunions most commonly occur in females but not because of the popular belief that they are caused from wearing high heels. High heels are undoubtably bad for almost every joint in your body including you big toe. However, I have known quite a few men with hallux valgus and I am almost 100% sure that they were not cross dressers! Once a bunion has formed wearing tight shoes (or high heels) will aggravate it and often causes redness, pain and swelling. The difficulty is that with this deformity many shoes will be too narrow to fit your wider foot.
There is a strong hereditary factor with bunions. However, the inherited disorder is usually one of connective tissue expressing ligamentous laxity and resulting in joint hypermobility. Joint hypermobility indicates a deficiency in the passive stabilisation system of the whole body. This condition overloads all the bony structures and in this case usually involves all the joints of the lumbar spine, pelvis, hips, knees and the feet. It is the laxity of the connective tissue in the feet that allows the first metatarsal of the big toe to wander medially leading to the valgus deformity [Fig. 1].
This problem starts at the pelvis. With their wider pelvis and increased Q-angle it is this factor that makes females at a higher risk of forming bunions. Our pelvis is the major control centre for our posture and inevitably effects the whole of the rest of the body. You will usually find a pelvic tilt in those with bunions. A pelvic tilt is highly correlated with an exaggerated lumbar lordosis, which affects abdominal wall strength and function. This in turn effects lower extremity posture and increases the incidence of injury to the lower extremities. The usual postural pattern with a hallux valgus is an anterior tilt of the pelvis (often one-sided), an internal rotation of the leg/knee, pronation of the foot and a big toe valgus.
It is important to start by correcting the pelvic tilt, with therapy if it is one sided. If bilateral you will need to simultaneously strengthen the abdominal muscles and the hip extensor muscles. This will contribute greatly to correcting your internally rotated legs and foot pronation. You can aid correcting the feet by practising walking with your toes lifted off the floor. The tendons of your inner arch belong to your toe extensors so strengthening them will help to strengthen the inner arch of your foot. Sensibly avoid tight shoes and high heels.
A condition that often accompanies hallus valgus and arises later on as a result of it is hallux rigidus. As the name suggests the deformed joint becomes degenerated and rigid. This is partially due to the compromised toe-off in the first stance of walking, and is exacerbated by the excess wear and tear of hypermobility. Rolling over the toes as we do when transiting from Rod to Upward Facing Dog is ideal to help in the prevention of hallux rigidus.
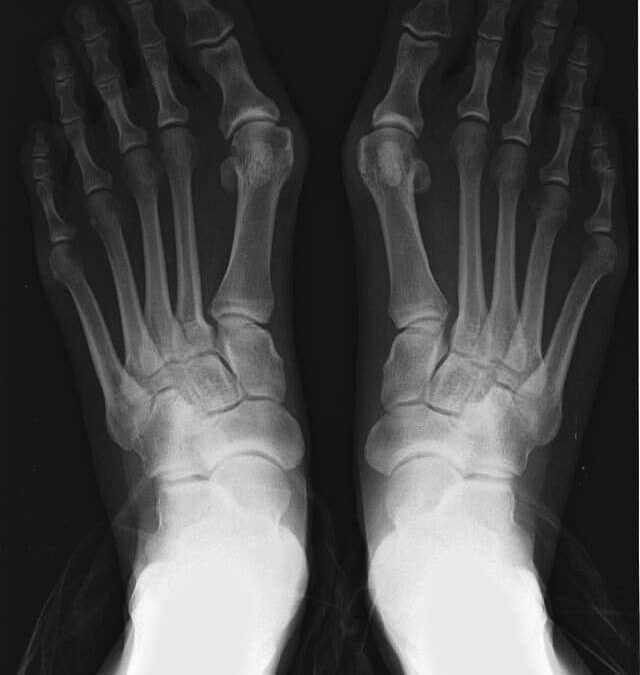
Figure 1: Medial deviation of metarsal bone with lateral deviation of phalanges.

Thanks for sharing a lot of very profound and interesting information in general on this blog and in your books.
Is there a coexistence between thyroid and hallux valgus?
Thanks Sandra
Thanks for you kind feedback Sandra.
I have never heard of these two particular conditions being linked. Have you?
Warmly
Monica
Thank you Monica for this very insightful article. I developed a bunion 2 months ago, in a whim, from one day to another.No hereditary factors but I have flat feet and am quite flexible, also carry chronic (light) sciatic, which from your article I understand may all relate to pelvis? ( although no obvious lordose).My question is : how can you prevent this condition from worsening further? Aren’t jumping back and chaturanga bad as they put weight on a misaligned toe? have you adjusted your practice? Or diet? Thank you in advance for your insights. I’ve been severely slowing down my practice not knowing how to handle this and you are the first ashtanga practitioner AND therapist really addressing specifically this issue , so your views are really valuable to me! 🙂
Hi Helen.
If you have sciatica there is definitely some dysfunction at your pelvis and/or low back. This coupled with your flexibility and flat feet are enough to create bunions. Note that the balls of the toes specifically relate to the psoas muscle which is usually involved in pelvis and low back issues. Also if you are very flexible as you age the feet tend to widen from the long-standing (pun : )) load on the ligaments there. The best you can do is to address your lumbopelvic problem with a holistic musculoskeletal specialist and preferably one who can give you some rehabilitative exercises. This will help to correct the your flat feet and if not, it would be worthwhile to address them specifically. Avoid hard orthotics, softer pliable ones are more effective. Both flat feet and bunions are usually symptoms of what is happening further up the kinematic chain.
Loading a deformed toe may increase the problem… I am unsure of that. The way we roll over the feet, however, does keep the toes flexible and prevent Hallux Rigidus which eventually usually accompanies Hallux Valgus.
I hope that helps Helen
Namaste
Monica
Thank you so much for your deep insights Monica! It does help indeed, they are accurate and I’ve planned to see an osteopath soon..
Namaste
Thank you, Monica, for this very insightful article. I always suspected that my flat feet, very flexible (often hyper flexible) lower back and my bunions were connected but I never had the anatomical explanation to back up my theories. I danced ballet for most of my childhood and adolescence, taught ballet for several years afterward and after two pregnancies my bunions grew quite severe, even though I retained flexibility in my feet. Over time, one foot began to hurt and as the pain got worse I decided to have a bunionectomy. Two years later (I did a yoga teacher training 5 months post-OP) I am very happy that I had the surgery. I have a regular Ashtanga practice and teach yoga, but recently my knee has started to hurt (on the non-operated foot). The second foot also has a substantial bunion but it does not hurt the way the 1st one did but I suspect (and I have a very good sense of my body) the bunion may be part of the knee pain. I am considering a 2nd bunionectomy because I have found it easier to have better alignment on the operated foot (especially in standing poses) even though the recovery is long (8 weeks before I could roll through on my foot) and painful. No matter how much I work on my arch, work on my pelvic alignment and do foot exercises, the bunion is so big that it works against my efforts. In your opinion, does it make sense to have a 2nd surgery for these reasons, even though the foot itself does not hurt so bad? Won’t a misaligned foot have consequences in the long run, even if it does not hurt now? Thank you and namaste.
Hi Rose
You are probably more qualified than me to answer if surgery is worth it as I have never had surgery on my bunions. Sometimes I wish I had!
What comes first, the chicken or the egg? No one knows. Certainly there is a kinematic relationship – no muscle works in isolation – so one might guess that the structural deformity of a bunion would at least perpetuate the cycle.
Your knee pain could of course be any number of things, facilitated lateral rotators or popliteus or an inhibited rectus femoris… Best is to get assessed by a good musclulsketeal professional.
Hope that is of some help.
Namaste
Monica
Hi Monica, thanks for sharing your knowledge on this topic. I seem to fit the picture of the anterior pelvic tilt, flat feet and bunions.
I started yoga three months ago and I am actually wondering if the sequences I am doing are right for me right now. I have more back pain than I used to have. Is there a sequence you could recommend to work on the anterior tilt and protect my lower back? Greetings, Famke
Hi Famke
From here it is impossible for me to tell if it is any particular posture or sequence of postures that you doing are causing you back pain, however, check that you are lengthening your spine in all postures versus exerting too much effort and then shortening your spine. The length needs to come from the waist down (pelvis descends downward) and from the waist up (crown of the head lengthens upward). Couple this with good bandha engagement and you will already be along way towards avoiding back pain by activating your core and creating space along the spine.
Additionally, the pelvis down action will help with your anterior tilt. The pelvis tilts anteriorly when the abdominal muscles are insufficiently strong.
I hope that helps.
Namaste, Monica
Hi Dr. Monica,
I have arthritis in my big right toe and now that toe is just starting to come over my second toe. Is there a yoga exercise that I can do to slow this down?
Thank you so muc.
Hi Annmarie
Apologies, my reply to this seems to have not been saved.
There are no specific yoga postures for this, however, you can focus on lengthening and spreading the toes to maintain mobility as well as rolling over the toes in vinyasas.
Apart form that you can do resistance exercises with thick rubber bands over the two joins in the big toes to activate and strenthen the muscles that oppose that inward pull.
I hope that is of some value…
Namaste, Monica
Thank you for this very interesting article. My bunions have improved significantly and are now virtually pain free since, with the help of a PT, I ditched my hard orthotics 2 years ago and started to work on toe extension & lumbricals, and walking barefoot ( which was uncomfortable at first). I also favor wide toe box trainers with flexible soles.
Just wondering, is there a typo in the 2nd sentence? My understanding of a valgus deformity is a movement of the distal end of the bone away from the mid line, not towards it.
I also LOVE your articles on sacral nutation and engaging lute max in backbends. As a trainee yoga teacher they are so helpful. Thank You!
Thank you Sue for the positive feedback. It is appreciated.
Perhaps I refer to valgus differently as I am referring to the metatarsal rather than the great toe itself as it is actually the movement of this bone that then causes the big toe to move towards the midline. Thank you for the clarification.
Namaste
Monica